Dr. Scott Naftulin D.O. and Dr. Bruce Zhang provide basic answers to frequently asked questions involving pain, treatment & therapy.
Dr. Naftulin and Dr. Zhang are physician partners of Northeastern Rehabilitation Associates (NERA) and specialists in pain associated with musculoskeletal & neurological conditions
Contact your doctor to diagnose your specific situation or make an appointment with Dr. Naftulin or Dr. Zhang and the NERA Specialty Spine associates to evaluate your medical condition.
In pain and can’t work? Whether this is a new or chronic problem, work-related or not, Physiatrists are trained to manage issues that may interfere with one’s ability to work.
Low back pain is the leading cause for disability world wide and account for at least one third of work related injuries. This lost work causes financial burden to both the individual and also the employer.
For work-related conditions, we manage work restrictions to try to keep our patients in the work force without inducing further harm. We strive to return to patients to work as safely and quickly as possible.
For more chronic conditions, applying for disability benefits can be very overwhelming. Your doctor can help you determine whether short-term, long-term, or social security disability is appropriate. We assist also by providing medical records and completing necessary paperwork (including FMLA and Social Security Disability evaluations).
Chronic pain is a complex medical condition that involves a multidisciplinary approach to treatment.
Pain can be treated by specialists in Physiatry (Physical Medicine and Rehabilitation), Anesthesiology, Interventional Radiology, or Physical Therapy. As a Physical Medicine and Rehabilitation practice, we treat not only the painful problem, but we treat the patient as a whole. We treat pain associated with any musculoskeletal problem and sub-specialize in spine pain/neck and back pain.
Pain Management does not only involve treating pain with medications. Although medications are often used to control symptoms, other options are often employed to minimize pain with possibly less side effects. Often when someone presents with pain, if there are no concerning signs or symptoms, conservative treatment is initiated. This often begins with a course of Physical Therapy or sometimes chiropractic treatments. Some medications may also be trialed during this time to minimize acute discomfort. If conservative treatment fails, it is often suggested to get advanced imaging studies (MRI, CT scan) if not already done to help diagnose the problem. Thereafter, interventional therapy may be offered.
Interventional therapies include diagnostic and therapeutic injections (with and without steroids/cortisone) into the spine or joint. Spinal injections are precise injections done under fluoroscopy (live X-ray) and consist of epidural steroid injections (selective spinal nerve blocks) or medial branch blocks (facet joint injections). This may consist of a single injection, but some are also done as part of a ‘series’ to be determined by your personal outcome and doctor’s preference. The majority of patients find some or total relief with these injections. Those that do not respond to conservative and interventional therapies may be referred to a surgeon for other treatment options.
Already have back surgery? Were you told there was nothing else that could be done? Patients who have failed back surgeries historically were told they had to ‘live’ with it. In more recent years, new therapies are being explored and discovered with ongoing technological advancements. Spinal cord stimulators are devices that can be implanted in the spine and offer relief for a variety of neuropathic pain complaints. Although this treatment may not work for everyone, many patients report 50-70% reduction in overall pain and have been able to lessen or cease use of pain medications.
Whether your pain is acute or chronic, it often interferes with your ability to work. Lower back pain is one of the most common causes for disability and work-related injuries. As physiatrists, we also manage disability with work restrictions, etc, with hopes of returning our patients back to gainful employment.
– Spine-Health.com. Pain Management Specialists. Accessed 11/04/2015.
– Spine-Health.com. Spinal Cord Stimulation for Chronic Pain. Accessed 11/04/2015.
Neuropathic pain comes in many forms and typically results from damaged nerve tissue or compressed nerves.
Nerve roots compressed from the spine usually cause cervical or lumbar radiculopathy (sciatica), as well as pain after back surgery (failed back syndrome). Other causes of nerve pain (usually from peripheral nerves) include nerve entrapment (i.e. Carpal tunnel syndrome), peripheral neuropathy (most likely from diabetes), phantom limb pain, or complex regional pain syndrome (CRPS), previously called RSD (reflex sympathetic dystrophy).
Neuropathic pain is typically described as:
- Severe, sharp, electric shock-like, shooting, lightning-like, lancinating
- Deep, burning or cold
- Persistent numbness, tingling, or weakness
- Radiating to the arms, hands, legs or feet
Diagnosing and treating nerve pain can be very difficult. Often electromyography and nerve conduction studies (EMG/NCV) are used to detect nerve damage and differentiate between nerve degeneration (neuropathy) and nerve root compression (radiculopathy).
There is no known cure or proven treatment for neuropathic pain. Treatment is instead focused on alleviating the pain caused by a painful nerve.
In cases of nerve entrapment, often times surgery is offered and may resolve all or most of the nerve pain symptoms. Treatment of nerve pain related to spine problems often requires a comprehensive treatment approach. Therapies often involve a combination of medications, nerve blocks, physical/occupational therapy, electrical stimulation (i.e. TENS units or implantable nerve stimulators) as well as psychological therapy.
– Spine-Health.com. Treatment Options for Neuropathic Pain. Accessed 11/02/2015.
Musculoskeletal pain affects not only bones and muscles, but also ligaments, tendons and nerves.
This pain can be caused by an acute injury, such as falls, fractures, sprains, dislocations, car accidents, and direct muscle trauma. It can also be a chronic condition, most commonly affecting the lower back. Joint pains from arthritis are also a common musculoskeletal complaint causing chronic pain.
Diagnosing musculoskeletal pain will depend on the cause, body part affected, and whether it is an acute or chronic condition. After taking a full medical history and physical exam, other diagnostic tests may be needed. These tests may include: blood tests, X-rays, CT scan or MRI.
Once the problem is diagnosed, appropriate treatment will be prescribed. In more acute conditions, your doctor may suggest starting with conservative treatment such as RICE (rest, ice, compression and elevation). Thereafter Physical/Occupational Therapy may be prescribed. Certain conditions may also benefit from temporary splinting of an affected joint to allow healing. Anti-inflammatory medications (i.e. Ibuprofen and naproxen) are also commonly prescribed for acute injuries to help both pain and swelling. These medications are also used for some chronic conditions such as osteoarthritis. Other treatment options for musculoskeletal pain may also include massage, chiropractic, acupuncture, or injections.
Reference: Cleveland Clinic. Musculoskeletal Pain. Accessed 10/30/2015.
Physiatrists, or rehabilitation physicians, are medical doctors who:
- Are experts at diagnosing and treating pain
- Restore maximum function lost through injury, illness or disabling conditions
- Treat the whole person, not just the problem area
- Provide non-surgical treatments
- Explain your medical problems and treatment plan
- Work not only on treatment but also injury prevention
Rehabilitation physicians are nerve, muscle, and bone experts who treat injuries or illnesses that affect how you move. Rehabilitation physicians have completed training in the medical specialty Physical Medicine and Rehabilitation (PM&R). Rehabilitation physicians treat a wide range of problems from sore shoulders to spinal cord injuries. Their goal is to decrease pain and enhance performance without surgery.
Rehabilitation physicians take the time needed to accurately pinpoint the source of an ailment. They then design a treatment plan that can be carried out by the patients themselves or with the help of the rehabilitation physician’s medical team. This medical team might include other physicians and health professionals, such as neurologists, orthopedic surgeons, and physical therapists. By providing an appropriate treatment plan, rehabilitation physicians help patients stay as active as possible at any age. Their broad medical expertise allows them to treat disabling conditions throughout a person’s lifetime.
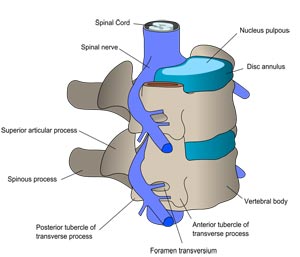
A disc herniation occurs when a portion of the inter-vertebral disc material bulges and ‘sticks out’ into the neural canal.
This can produce pressure on the spinal cord or nerve roots and cause pain, numbness, or tingling into the arm or leg. This is very rarely a surgical condition and usually responds with non-surgical treatment. This is also often referred to as a “slipped disc” or “ruptured disc” and can usually be treated without open surgery.
Related Articles / Suggested Reading
There are many causes of back pain including injury or trauma.
Common Causes of Back Pain Include:
- Muscle Strain
- Bulging or herniated disc
- Degenerative disc disease
- Spinal stenosis
- Sciatica or pinched nerve
- Sacroiliac joint
- Facet (zygapophyseal) joint
- Arthritis
There are also many other conditions which can contribute to back pain. These conditions are almost always treated non-surgically, resulting in a successful outcome the vast majority of the time.
Related Articles / Suggested Reading: Back Pain (Upper & Lower Back) – Assorted articles from the doctor regarding diagnosis, treatments and procedures.
The sacroiliac (SI) joint can cause pain in the low back or buttocks. This is especially common in women, and often radiates into the leg, masquerading as sciatica. SI joint pain generally responds well to non-steroidal medications and physical therapy. Occasionally, injections into or around the joint space are necessary to completely alleviate the pain and dysfunction and clarify the diagnosis.
Related Articles:
The epidural steroid injection is the placement of cortisone, a powerful anti inflammatory agent, into the epidural space, which approximates the disc and spinal column.
The treatment of epidural injection has been around for over 40 years. It involves using either steroids or anesthetic agents allowing good benefit with minimal risk. The main goal of the epidural injection is to decrease any inflammation or pain resulting from disc problems, arthritis, or stenosis, which may be irritating a spinal nerve.
Pain or a ‘pins and needles’ sensation can sometimes be present in the arms, hands, legs, or feet. There are many items that cause these symptoms, including:
Carpal Tunnel Syndrome
Carpal tunnel syndrome is a hand and arm condition that causes numbness, tingling and other symptoms. Carpal tunnel syndrome is caused by a pinched nerve in your wrist.
Related Articles
- Carpal Tunnel Syndrome (CTS) – Symptoms, Diagnosis & Therapy
- Peripheral Nerve Stimulation (PNS)
- Electromyogram (EMG) & Nerve Conduction Studies (NCS)
Peripheral Nerve Damage
A herniated or inflamed disc in the disc can irritate or compress a nerve that travels into the arm or leg, and thereby produce symptoms of pain, numbness, or tingling. The symptoms can sometimes go from one extremity to another. Although this may cause alarm, there are many non-surgical treatment options available.
Related Articles
MRI or Magnetic Resonance Imaging, is a type of powerful radiographic study that provides a clear diagnostic picture without using radiation. The MRI image gives enhanced views of the body part in question. An MRI scan of the spine, for example, provides a superior view of the discs in the back, as well as the nerves and other soft tissues.
The doctor can look at the MRI films and determine whether there is a pinched nerve, a degenerative disc, a tumor, or in some cases spinal stenosis. The doctor may use the MRI to correlate with the patient’s symptoms and physical exam.
The greatest advantage of the MRI is in its ability to allow the physician to see inside the body without the need for surgery or potentially harmful radiation.
Steroids are very effective in decreasing swelling and inflammation in the body. Often steroids are used to ‘cool off’ inflammation in a joint or in the spine around a disc. This is a very effective treatment method with few side effects.
Many patients ask about the potential risks or side effects of steroid use. While it is true that long-term repetitive use of steroids over many years can increase the risk of side effects, short-term cortisone use in the form of injections or oral medications is thought to be relatively safe with hardly any side effects or problems. Be sure to ask your doctor if you have any questions or concerns, please contact us for a consultation and appointment.
No. Our physicians, physical therapists and professional staff treat all kinds of patients with all kinds of injuries.
Athletes and non-athletes alike receive the same level of care and service, and we treat each patient based on his or her individual condition and goals.
Whether you a weekend gardener or duffer, a high school or collegiate intramural player, a pro athlete or a total non-athlete, we will work to diagnose your condition and work to relieve you of pain in a manner consistent with your activity needs and goals.
When athletes or active adults are hurt, they look for comprehensive treatment that will help return them to their sports or activities as quickly as possible.
We have built years of experience in sports-related injuries and conditions related to physical activity. We combine that expertise with state-of-the-art equipment and techniques and an integrative, team approach to care.
Physicians, physical therapists and professional staff work together to develop treatment and rehabilitation plans tailored to each patient and designed to achieve the most positive outcome.
Although rest may be indicated immediately after an acute injury, most musculoskeletal injuries will recover faster with controlled activity.
It is essential to make a correct diagnosis before determining the amount and duration of rest and activity. With a physician-directed rehabilitation program, your recovery will be facilitated and optimized so that you can return to your pre-injury lifestyle including vocational and avocational activities and minimizing the risk for re-injury.
We recommend ice for the first day or two after you suffer an acute injury.
Applying ice helps reduce circulation, which, in turn helps decrease the amount of swelling after an injury. An easy reminder for reducing swelling and pain is RICE Rest, Ice, Compression and Elevation. You can use moist heat after the first 72 hours to increase the blood flow to the injured area to reduce pain and stiffness.
For more chronic injuries, the use of ice or heat depends on the injury and response to therapy. We always caution patients to never use a heating pad in bed as even on low heat settings severe burns can occur.
If you can not put your weight on the injured limb after an injury or by the time you see your doctor, he or she will probably order an X-ray.
See your doctor if you have persistent pain, swelling, discoloration or a locking or catching sensation. For an injury assessment, call us at 610-954-9400
or email us on-line to make an appointment.
Returning to normal activity depends upon many factors.
Our specialists evaluate each patient based on his or her injury and goals, and then develop a treatment and rehabilitation plan designed to return patients to physical activity safely and at the right time to help avoid re-injury.
We treat a variety of injuries and conditions, ranging from sprains and strains to more severe injuries such as ligament ruptures, joint instabilities or chronic degenerative conditions like arthritis. We also treat work and industry-related injuries, as well as injuries resulting from auto accidents.
Your doctor may refer you to us for treatment, or you can call Specialty Spine Care at 610-954-9400 if you have pain or discomfort that limits your everyday or recreation activities or if you’ve just experienced acute trauma, a fall or an accident.
Contact us by email on-line for a Consultation Injury Assessment and Appointment.