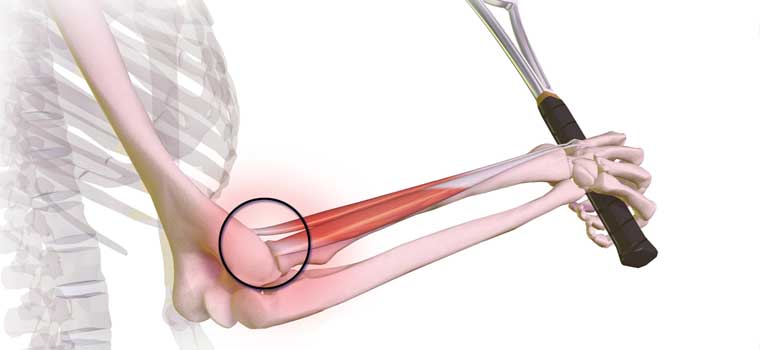
Epicondylitis is a type of tendinitis, or inflammation of the tendons, affecting the elbow causing pain in the elbow and forearm.
There are two types of epicondylitis: Tennis elbow affects the tendons on the outer side (lateral epicondylitis), where golfer’s elbow (medial epicondylitis) affects tendons on the inner side of the elbow. Both are very similar in terms of causes, symptoms and treatment.
Tennis Elbow
Tennis elbow is the more common type and as the name suggests is common in tennis players as well as other racket sports. However, you can get tennis elbow a number of other ways as well including repetitive gripping, especially if using the thumb and first two fingers. It is commonly seen in carpenters, plumbers, typing, painting, raking, weight lifting, knitting and similar activities that put repetitive stress on the tendons in the elbow. Pain may be elicited by lifting, making a fist or gripping, opening a door, shaking hands and other movements that extend the wrist.
Golfer’s Elbow
Golfer’s elbow is similarly caused by repetitive stress and not only found in golfers. This condition is usually caused by overusing muscles that grip, rotate the arm and flex the wrist. Improper lifting, throwing, swinging or poor conditioning during activities such as racket sports, weight lifting, bowling and baseball (also called pitcher’s elbow) as well as professions like carpentry and plumbing can also be associated with higher risks. Pain is often elicited by gripping and other symptoms may include weakness, stiffness as well as numbness or tingling radiating into fingers.
Treatment of Epicondylitis
Initial conservative treatment is focused on relative rest, avoiding activities that cause pain, ice, anti-inflammatory medications, bracing, stretching and strengthening. Using proper equipment and body mechanics are also important to prevent recurrent episodes. Symptoms will usually resolve spontaneously.
Injections: Both steroid injections as well as Platelet-Rich Plasma (PRP) are commonly used in the treatment of chronic epicondylitis.
Studies have shown that steroid injections showed more favorable outcomes in the short term (4- and 8- weeks); but PRP showed improved pain and function over steroids in the long term (24 weeks). Other studies have shown significant and sustained improvement often with just a single PRP injection that is considered safe and effective and has significantly reduced the need for surgery.
PRP is a procedure performed in the office using a patient’s own blood. Blood is drawn, like a simple blood draw, and then separated by centrifuge. The PRP is then drawn into a syringe and re-injected into the targeted area using imaging guidance (in this case – ultrasound). By using a patient’s own blood, we avoid the risk of cross-reaction, rejection and disease transmission.
PRP induces a healing reaction, or inflammatory response, which may temporarily increase pain for usually no more than 1-2 weeks. Anti-inflammatory medications, such as Ibuprofen, must be avoided for a short duration both before and after the injection to allow the inflammatory reaction to initiate the healing process. This process may take weeks to months to see the intended benefits. The PRP can be given alone or mixed with other regenerative tissues or chemicals in an effort to maximize the healing response.
Although steroids can be very effective for inflammation, they come with their own risks. Steroids are commonly known for systemic reactions which may be minor, such as increased appetite, mood changes, facial flushing, headaches and insomnia; or more severe, such as weight gain/fluid retention, hyperglycemia, bone loss, or thinning/fraying/rupture of a tendon, muscle atrophy or necrosis. Steroids may potentially worsen the condition over time, whereas PRP may reverse it.